
Pelvic girdle pain (PGP), also known as pelvic pain, is a common problem among women during pregnancy and postpartum that physiotherapists treat. However, it can also affect men and women who have not gone through pregnancy. Pelvic girdle pain can have a significant impact on daily life and can be challenging to manage. In this blog post, we will discuss the causes, symptoms, and treatment options for pelvic girdle pain.
What is Pelvic Girdle Pain?
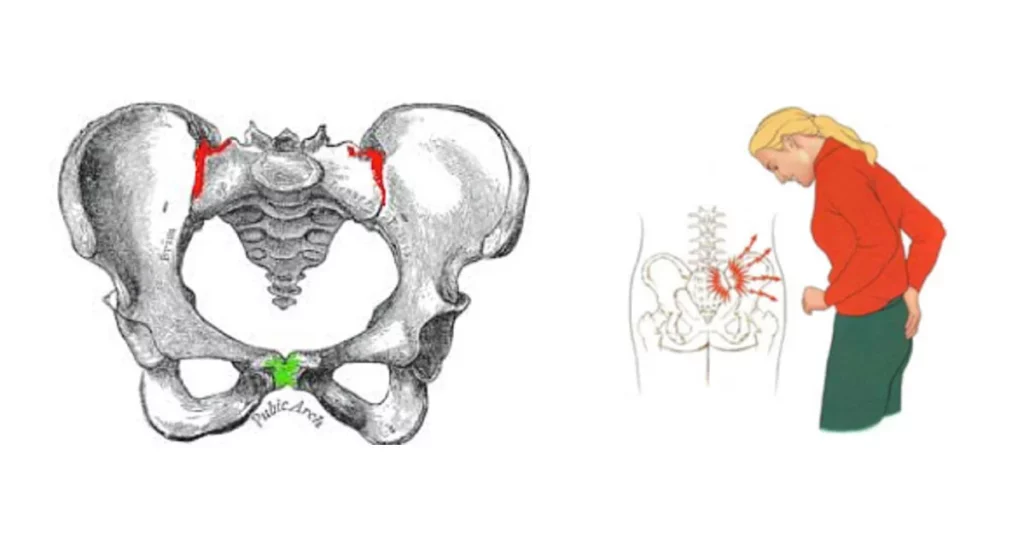
The pelvic girdle consists of the bones, ligaments, and muscles that connect the spine to the lower limbs. PGP refers to pain in the lower back, hips, groin, and thighs that is caused by dysfunction or instability of the pelvic joints. This pain can range from mild discomfort to severe, debilitating pain that affects daily activities.
Causes of PGP
There are several causes of PGP, including:
- Pregnancy: During pregnancy, the hormone progesterone is released, which softens the ligaments and joints in the pelvic area to prepare for childbirth. This can lead to instability and pain in the pelvic girdle.
- Trauma: A fall, car accident, or sports injury can cause trauma to the pelvic girdle, leading to pain and dysfunction.
- Arthritis: Arthritis is a condition that causes inflammation and pain in the joints, including those in the pelvic girdle.
- Muscle imbalance: Weakness or tightness in the muscles around the pelvic girdle can cause dysfunction and pain.
Symptoms of Pelvic Girdle Pain
The symptoms of PGP vary from person to person but can include:
- Pain in the lower back, hips, groin, and thighs
- Stiffness in the lower back and hips
- Difficulty walking, climbing stairs, or standing up from a seated position
- Pain during sexual intercourse
- Incontinence or difficulty urinating
- Numbness or tingling in the legs
PGP Assessment
The first step in physiotherapy treatment for PGP is an assessment. The physiotherapist will conduct a thorough examination to assess the range of motion, strength, and stability of the pelvic girdle. They may also use special tests to diagnose the specific problem and rule out other conditions that may be causing the pain.
Physiotherapy Treatment
Once the assessment is complete, the physiotherapist will develop a customised treatment plan that may include one or more of the following:
- Exercises: Exercises can help improve the strength and stability of the pelvic girdle muscles. This can include a combination of strengthening, stretching, and stabilisation exercises. Strengthening exercises may include squats, lunges, and bridges, while stabilisation exercises may include pelvic floor muscle exercises and core strengthening exercises.
- Manual therapy: Manual therapy involves hands-on techniques to help reduce pain and improve joint mobility. This may include massage, joint mobilisation, and manipulation.
- Education: The physiotherapist will educate the patient on proper posture, body mechanics, and safe lifting techniques to help prevent further injury.
- Supportive devices: A pelvic support belt or crutches may be recommended to provide support to the pelvic girdle and reduce pain.
- Modalities: Modalities such as heat, ice, ultrasound, or electrical stimulation may be used to reduce pain and inflammation.
- Progression: As the patient progresses, the physiotherapist may increase the intensity and complexity of the exercises to further improve strength and stability.
- Collaboration: The physiotherapist may collaborate with other healthcare professionals, such as a doctor to provide comprehensive care.







