What to Expect After 2 Weeks of Physiotherapy?

Key Takeaways
- By week 2, most patients notice small but meaningful changes — slightly less pain, better movement, and more confidence — while major strength and tissue changes are still developing beneath the surface.
- Mild post-exercise soreness is completely normal at this stage, but sharply worsening or unrelenting pain should be discussed with your physiotherapist.
- Consistency with your home exercise program (around 3–4 times per week) is the main predictor of progress by week 2, more than how “hard” each session feels.
- Recovery is rarely linear; some up-and-down days are expected, and week 2 is about building habits and trust in your treatment plan, not achieving full recovery.
- At Head2Toe Physiotherapy & Podiatry, we use structured, evidence-based progress reviews around the 2–3 week mark to ensure your recovery journey stays on track.
Starting physiotherapy is an important step towards better physical health. But by the two-week mark, many patients find themselves asking: “Am I improving enough?” or “Is this normal?” These questions are completely valid. The truth is, week two is less about dramatic results and more about building the foundation for long-term progress. Let’s break down exactly what you should expect.

Where You Should Be by the End of Week 2
By day 10–14 of physiotherapy — usually after 3–5 sessions for most patients — the goal is early adaptation rather than complete recovery. This is true whether you’re managing a minor injury or working through post surgical rehabilitation.
For common issues we see at our Melbourne clinics, here’s what most patients typically notice by week 2:
- Lower back pain: Slightly easier getting out of chairs, less stiffness first thing in the morning
- Knee pain: Walking and stairs feel marginally easier, the “sharp” edge to pain is dulling
- Post-ankle sprain: Better weight-bearing, reduced swelling, more predictable discomfort patterns
- Post-surgery: Early movement milestones being met, surgical site healing progressing
Some patients may feel only subtle change, especially with long-standing problems. If you’ve had chronic neck pain for 18 months, don’t expect a complete turnaround in 14 days — and that’s completely normal at the two-week mark.
For acute injuries like a rolled ankle from a weekend game at Princes Park or Clifton Hill, pain and swelling should usually be trending down with better weight-bearing by week 2. For chronic conditions like desk-related neck pain from working in the CBD, improvements might show more as better posture awareness and slightly longer “good” periods, rather than constant relief.
How Your Body Is Adapting in the First Two Weeks
“Early adaptation” describes how your tissues, joints, and nervous system start responding to the new loading and movement patterns introduced by physiotherapy. During this phase, your body is literally rebuilding and reorganising at a cellular level through a process called mechanotransduction.
Common physical sensations at this stage include:
- Mild muscle soreness 12–48 hours after exercises (delayed-onset muscle soreness typically peaks at 24–48 hours)
- A “worked” feeling in muscles rather than sharp pain
- Occasional temporary increases in stiffness after trying new movements
- Slight improvements in range of motion, often from 0-90 degrees towards 0-95 or beyond depending on your condition
Your nervous system is also beginning to “down-regulate” pain in previously sensitive areas. You might notice you can sit a bit longer before back pain kicks in, or lift a shopping bag with less guarding and apprehension. Research shows neural drive improvements of 20–30% can occur in these early weeks, particularly when combined with targeted quad activation exercises.
At Head2Toe, manual therapy techniques like joint mobilisation, soft tissue work on affected areas including quads, IT band, and Hoffa’s fat pad, or dry needling when appropriate, help settle symptoms and improve joint movement. However, long-term change comes from repeated, graded exercise — the hands-on work creates a window for you to move better.
Brief flare-ups after increasing exercise volume are often normal feedback. But persistent or severe spikes in discomfort should prompt a conversation with your therapist.
What Happens in Your Week 2 Physio Sessions
By the second week, sessions at Head2Toe start shifting from primarily assessment and symptom relief towards refining technique and gently progressing load. Your first physiotherapy appointment focused heavily on your medical history and initial assessment — now it’s time to build on that foundation.
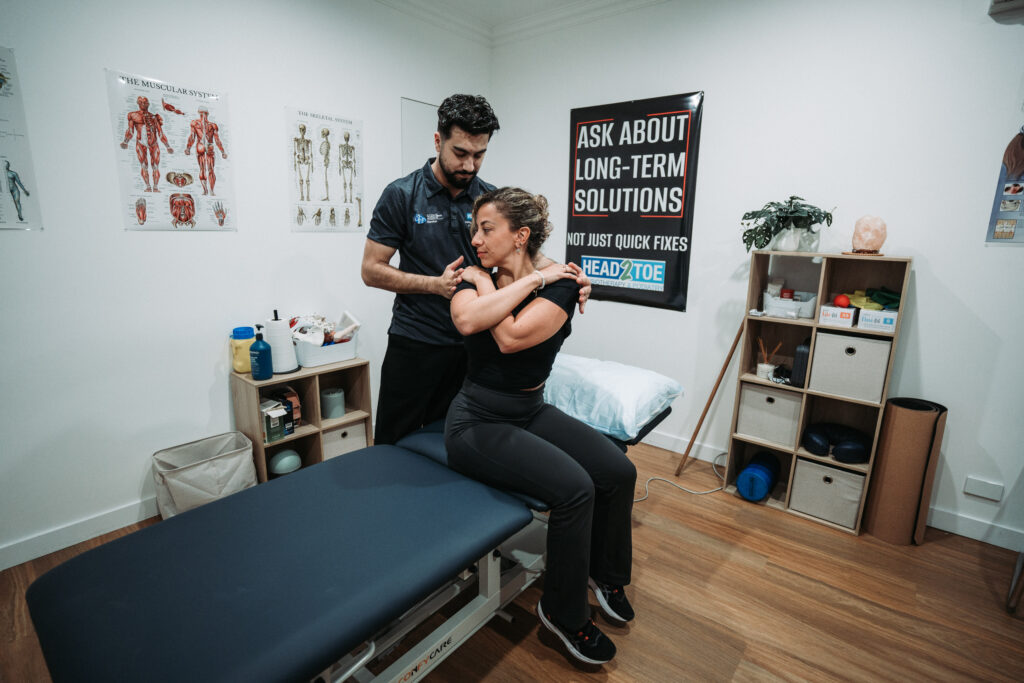
During your physiotherapy appointment, your physiotherapist will typically:
| Focus Area | What Happens |
|---|---|
| Objective assessment | Re-checking key measures from week 1 (knee bend angle, shoulder elevation, lumbar flexion) |
| Manual therapy | Hands-on treatment including massage, joint mobilisation, soft tissue work |
| Targeted exercises | Bodyweight squats, band work, balance drills, controlled movement patterns |
| Education | Short segments about pain, healing timelines, and activity modification |
| Gait review | For lower limb issues, walking pattern assessment with cues around stride length and weight shift |
For suitable patients, this is often when clinical Pilates-style exercises may be introduced — such as gentle reformer work in small groups of up to 5 people — focusing on control rather than intensity.
Your physiotherapist’s role is to assess your progress, refine your exercises, and ensure you’re building strength safely. Each physiotherapy session builds on the last, creating a progressive pathway through your rehabilitation.
Your Home Exercise Program by Week 2
Your home exercises are the main “engine” of real progress between appointments. They’re usually prescribed from your first session, then refined by week 2 based on how your body has responded.
A typical week 2 program might include:
- 4–8 simple exercises such as heel raises, bridges, banded rows, pelvic floor activation, and posture breaks
- 10–20 minutes per session
- 3–4 times per week frequency
- Exercises like straight leg raises (often 3 sets of 10, three times daily), quad sets, heel slides, and short arcs
The focus should be technique quality over intensity: slow, controlled reps with clear breathing and no rushed movements. Think 30-second breaks between sets, not powering through exhausted.
Practical habit-building tips for busy Melbourne professionals:
- Pair exercises with morning coffee
- Complete a quick session during a 5–10 minute break from your laptop
- Do gentle exercises in the evening before TV
- Stack the habit with something you already do daily (like after brushing teeth)
If any exercises consistently cause pain above your pre-agreed threshold — for example, more than 3–4 out of 10, or discomfort that lingers for hours — report this so we can adjust your personalised treatment plan.
Pain, Soreness, and What’s “Normal” at Two Weeks
Complete pain relief is uncommon by week 2, especially for significant injuries, acute injuries, or post-surgical cases. This doesn’t mean physiotherapy treatment isn’t working.
Here’s how to distinguish between acceptable and concerning symptoms:
| Normal Post-Exercise Soreness | Concerning Pain |
|---|---|
| Dull ache in worked muscles | Loss of nerve/bladder/bowel control |
| Resolves within 24–48 hours | Pain that escalates and doesn’t settle |
| Improves with gentle movement | Significant new swelling |
| Predictable pattern | Night pain that wakes you |
Many patients notice their symptoms becoming less intense and less constant by day 10–14, even if they still appear with certain tasks like sitting at a desk for 2+ hours or walking up hills in Brunswick or Kew.
Stress, poor sleep, and busy work periods — like end-of-month deadlines — can temporarily heighten sensitivity. This doesn’t mean your physiotherapy sessions aren’t working. Your nervous system simply has less capacity to filter signals when you’re run down.
At Head2Toe, clinicians proactively discuss pain expectations, acceptable discomfort ranges, and simple strategies for managing pain including cold therapy, heat application, and gentle mobility breaks throughout your daily activities.
Why Consistency Beats Intensity at Week 2
Research and clinical experience consistently show that doing your prescribed program regularly matters far more than occasional intense efforts. Data from rehabilitation cohorts shows patients adhering to 3–4 physiotherapy sessions weekly progress 25–40% faster in range of motion and strength metrics.
By week 2, the focus is on building reliable habits:
- Showing up to appointments
- Completing home exercises
- Following activity modification guidelines
- Tracking your progress
Consider this contrast: A patient doing 10–15 minutes of targeted gentle exercises most days tends to progress faster than someone who does a single long, exhausting session once a week. The former also experiences approximately 50% fewer flare-ups by week 6.
Simple accountability methods that work:
- Printed tick-box sheet on the fridge
- Phone calendar reminders
- Notes in a habit-tracking app (research shows 85% compliance with apps versus 60% paper-based)
- Setting reminders tied to your daily commute
Communicating barriers honestly — long days in the office, school drop-offs, fatigue — allows your physio to simplify or adjust the plan so it remains realistic rather than abandoned. Around 30% of patients drift away from their programs without tracking, leading to twice the dropout rate by month three.

How We Measure Progress at Head2Toe
At around the 2-week mark, Head2Toe physiotherapists start comparing objective assessment measures and patient-reported outcomes against your baseline from your first week.
Common metrics we track include:
- Range of motion: Degrees of knee bend, shoulder elevation, spinal flexion
- Strength tests: Single-leg calf raises, grip strength, quad contraction scoring
- Functional tasks: Sit-to-stand repetitions in 30 seconds, step-downs, balance times
- Outcome questionnaires: Standardised tools measuring function and symptoms
Subjective wins are equally important in tracking your recovery:
- Better confidence on stairs at Moonee Ponds station
- Fewer painkillers needed during the day
- Being able to sleep through the night more often
- Walking 15–20 minutes daily without significant flare-ups
- Reduced reliance on activity modification
If clear progress isn’t evident by the end of week 2–3, we’ll review the diagnosis, loading strategy, and any contributing factors like footwear, workplace setup, or training volume. This structured, evidence-based review helps keep your treatment plan on track.
For patients where foot and ankle biomechanics are affecting recovery, collaboration with Head2Toe podiatrists ensures we address the complete kinetic chain. Physiotherapy helps most patients when combined with this integrated approach to function and mobility.
Common Setbacks and How to Handle Them
Many patients experience at least one minor setback or flare-up in the first fortnight. Research shows 70–80% of cases demonstrate plateaus or minor regressions around day 10–14 due to fatigue accumulation. This is normal.
Typical scenarios that trigger setbacks:
- An extra-long walk along the Yarra
- A full weekend of gardening
- Lifting heavy boxes when moving house
- Returning to social sport a bit too early
- Sudden increases in sitting time at work
Your simple flare-up plan:
- Reduce intensity for 24–72 hours
- Switch to gentler exercises from your program
- Use symptom relief strategies (ice, heat, gentle mobility)
- Contact your physio if pain doesn’t settle within a few days
Don’t abandon your program after one bad day. Setbacks provide valuable information to refine load and expectations. Overload risks approximately 10–15% setback rates, so prevention through pacing is key.
At Head2Toe, clinicians educate patients on recognising patterns that precede flare-ups — cumulative hours sitting, sudden spikes in running distance, footwear changes, or scar tissue sensitivity — to reduce recurrences and support prevention of future issues.
Looking Ahead: What Weeks 3–4 Usually Bring
The most noticeable functional gains for many health conditions occur between weeks 3 and 6, building on the foundation you’ve established in the early weeks. Week 2 focuses on adaptation; weeks 3–4 bring real progress in function and mobility.
If week 2 has gone well, your physiotherapist may gradually increase load:
- More repetitions per exercise
- Slightly heavier resistance bands or free weights (ankle weights on SLR, eccentric quads)
- More challenging balance and control drills
- Step-ups, wall squats, leg press progression
- Sport-specific movements where appropriate
For many patients, this is when daily life activities become increasingly manageable — carrying shopping, climbing stairs, or cycling short distances around Melbourne. Goals like full active range of motion, normalised gait, and eventually return to running (typically by week 8) become achievable.
Some individuals may transition into or increase clinical Pilates, sport-specific drills, or work-conditioning tasks depending on goals. Whether you’re aiming for return to running at Princes Park or pain-free office workdays, the pathway becomes clearer.
The overarching aim at Head2Toe is not just short-term symptom relief but sustainable capacity — helping you get better, stay better, and live better with lasting improvement in your physical therapy outcomes.

When to Contact Your Physiotherapist Before Your Next Appointment
Open communication is essential, especially in the early weeks of your recovery journey. You should never feel you’re “bothering” the clinic by asking questions between sessions.
Contact us if you experience:
- Rapidly increasing pain over several days
- New unexplained swelling in the affected area or surgical area
- Loss of movement compared with week 1
- Pain disturbing sleep most nights
- Uncertainty about exercise technique
- Pain in an unexpected area during exercises
- Missing several days of exercises due to workload or family commitments
Motivation or adherence struggles are just as important to discuss as symptoms. If your schedule has changed or life has gotten busy, let us know so we can simplify your program rather than watching it get abandoned.
Head2Toe offers one-on-one consultations in private rooms, allowing time for thorough review and modification of programs if any concerns arise. Early communication prevents approximately 30–40% of setbacks according to longitudinal studies — so don’t wait for your next scheduled appointment if something feels wrong.
Ready to stay active and continue making progress? Book an appointment today to ensure your recovery stays on track.
FAQ
Is it normal if I don’t feel much better after two weeks of physiotherapy?
For long-standing problems — such as chronic lower back pain present for 6–12 months — only subtle improvements may be visible by day 10–14. You might notice slightly easier movement, fewer severe pain spikes, or better tolerance for sitting, but not dramatic change. This can still be completely appropriate. Many meaningful strength and tissue changes take 4–12 weeks of consistent loading to become apparent. However, if there’s absolutely no change at all by week 2–3, this is a good time to review goals, technique, and diagnosis with your physiotherapist.
How many physio sessions will I usually have in the first two weeks?
Most patients at Head2Toe attend around 1–2 physiotherapy sessions per week in the early phase, meaning by the end of week 2 you’ve typically had 2–4 appointments. Frequency may be higher for acute post-surgical rehabilitation or significant sports injuries, and lower for milder or more chronic issues. The exact schedule is individualised based on condition severity, your goals, and how independently you can manage your home exercise program between visits. One session per week works well for many patients with established routines.
Can I keep working or exercising while I’m in week 2 of physio?
Many people in Melbourne continue office work or light duties while undergoing physiotherapy, with appropriate modifications to posture, breaks, and load. Low-impact exercise such as gentle walking, stationary cycling (10 minutes on a stationary bike is often encouraged by week 2–3), or basic Pilates is frequently recommended, provided it doesn’t significantly flare symptoms. Return to higher intensity sports — football, netball, long-distance running — usually requires explicit clearance and a graded plan from your physiotherapist to reduce pain risk and prevent re-injury.
What if my pain feels worse after starting physio exercises?
A temporary increase in soreness when first loading deconditioned tissues is common, especially in the first week or two. Physiotherapy techniques intentionally challenge your body to adapt. Warning signs that pain is excessive include severe spikes, symptoms that don’t ease within 24–48 hours, significant swelling, or loss of function you previously had. Contact your Head2Toe physiotherapist promptly so exercises can be modified, dosages adjusted, or alternative strategies trialled. Remember, reducing inflammation and managing early discomfort is part of the process.
Do I need imaging (X-ray or MRI) if I’m still sore at week 2?
Many musculoskeletal issues improve with conservative care and don’t automatically require imaging at the 2-week point. Your physiotherapist will screen for red flags — such as significant trauma, marked weakness, or systemic symptoms — that might prompt referral for scans. Decisions about imaging are made case-by-case, often in collaboration with GPs or specialists when indicated. In many cases, what we find on scans doesn’t change the rehabilitation approach, so we focus on functional improvement and symptom response first.







