Key Takeaways
- After your first session at Head2Toe Physiotherapy & Podiatry, you’ll leave with a clear diagnosis, a treatment plan, and typically specific therapeutic exercises to start on.
- The first 1–2 weeks are an adaptation phase where mild soreness or fatigue is normal as your body adjusts to hands on treatment and new movement patterns.
- Most people with mild–moderate injuries notice measurable change within 2–4 weeks, while longer-standing issues often need at least 6–8 weeks of structured rehab.
- Doing your home exercises as prescribed (usually 3–4 times per week) and attending planned follow-up appointments is essential for progress.
- You can contact the clinic between sessions if pain changes, exercises feel unclear, or you’re unsure about activity levels.
Starting physiotherapy is a significant step toward recovery. You’ve completed your initial consultation, and now you’re wondering what happens next. At Head2Toe, your first physiotherapy appointment establishes the foundation—but it’s what you do in the days and weeks following that determines your results. Here’s exactly what to expect after your first visit.
What Happens Immediately After Your Initial Consultation
By the end of your first appointment you’ll understand your diagnosis, the root cause of your symptoms, and your next steps. This isn’t guesswork—it’s the result of a thorough physical assessment and physical examination.
Your physiotherapist will summarise key findings in plain language. For example, they might explain that your shoulder pain is driven by reduced rotator cuff strength, or that your lower back discomfort relates to stiff lumbar joints and poor body mechanics. This clear diagnosis helps you understand what’s actually happening rather than leaving with vague instructions.
You’ll receive both a short-term plan (covering the first 1–2 weeks) and a longer-term pathway (typically 6–8 weeks). This personalised treatment plan is usually provided in writing or sent via an exercise app or email. You won’t be left wondering what to do next.
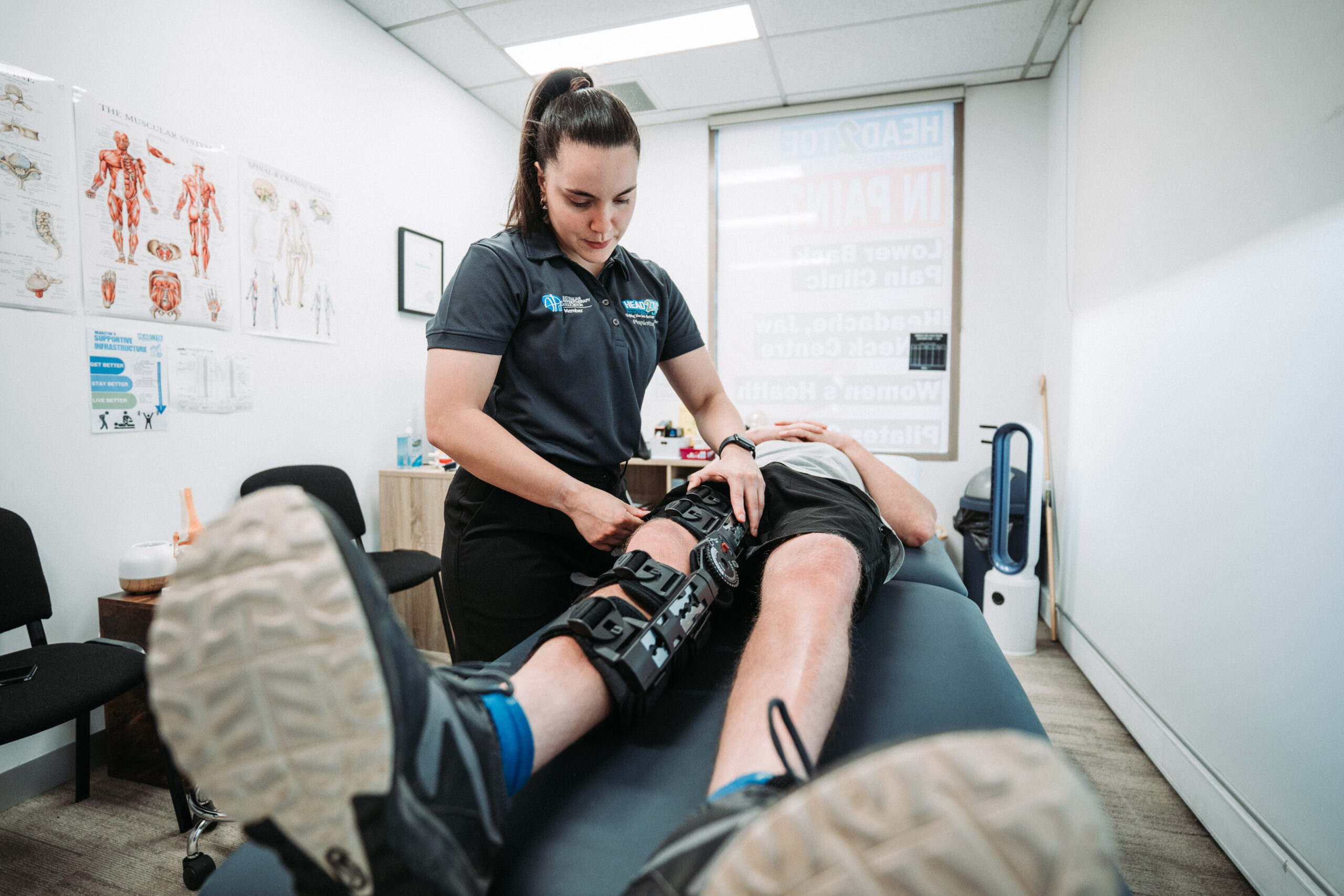
Initial hands on treatment often continues right up to the end of your first session. This might include joint mobilisation, soft tissue massage, dry needling, or taping—specific techniques selected based on your assessment findings. The session begins with evaluation and finishes with active treatment.
Before you leave the Moonee Ponds, Brunswick, Kew, or Pascoe Vale clinic, you’ll know when your next review appointment is scheduled. This structure ensures your recovery journey has momentum from day one.

The First 1–2 Weeks: The Adaptation Phase
The first 7–14 days after your initial consultation are about settling symptoms and helping your body adapt to new loads and movement patterns. This phase is critical, and understanding what’s normal can prevent unnecessary worry.
Common, normal responses during this phase include:
| Response | Duration | What It Means |
|---|---|---|
| Mild post-treatment soreness | 24–48 hours | Tissues responding to manual therapy techniques |
| Muscle fatigue from new exercises | First few sessions | Muscles being challenged in new ways |
| Increased awareness of the injured area | 1–2 weeks | Heightened body awareness (not worsening) |
These sensations usually indicate tissues are adapting—not that your injury is getting worse. However, if pain is sharp, escalating, and lasts more than 72 hours, raise this with your physiotherapist/
Unless told otherwise, aim to complete your home exercises around 3–4 times per week at a comfortable challenge level. Mild discomfort during exercises is acceptable; severe pain is not. Your physiotherapist will have discussed this threshold during your first physiotherapy session.
Patients are encouraged to stay generally active in daily life. Walking, office work, and light household tasks typically continue within the limits discussed with your health professional. Complete rest is rarely the answer—activity modification is usually more effective for recovery.
Your Home Exercise Program: What To Expect and How To Use It
Your home exercise program isn’t generic. It’s tailored to your diagnosis, current strength levels, and goals—whether that’s returning to running, playing with your kids, or achieving pain relief during office work. This is a key part of your tailored treatment plan.
During the initial consultation, your physio will demonstrate each exercise and provide clear instructions on sets, reps, tempo, and weekly frequency. Programs typically focus on building strength, control, and load tolerance rather than short-term stretching alone. These therapeutic exercises address the underlying problem, not just the symptoms.
If an exercise repeatedly causes a flare-up thats severe, stop that exercise and contact the clinic. Signs to watch for include:
- Pain above 6–7/10
- Increased swelling
- Symptoms that don’t settle within 24 hours
Practical tips for consistency:
- Set reminders on your phone
- Link exercises to a daily habit (e.g., after brushing teeth or morning coffee)
- Use a small home space—most exercises don’t require gym equipment
- Track completed sessions in a simple notebook or app
Your exercise program will evolve over your few sessions as you progress. What starts as basic control work may advance to more challenging movements as your body adapts.
Tracking Progress: What Improvement Usually Looks Like
Recovery is usually gradual and non-linear. You’ll have better days and worse days, but the overall trend should move upward over weeks. Don’t expect a straight line—expect a general direction.
General timeframe guide:
| Condition Type | Expected Timeframe |
|---|---|
| Mild–moderate injuries (recent ankle sprain, acute back strain) | 2–4 weeks for measurable change |
| Longer-standing issues (chronic pain, tendon problems) | 6+ weeks of consistent treatment |
| Complex or post-surgical cases | Variable; guided by your physio |
Progress markers extend beyond pain levels. Look for improvements in:
- Sleep quality (less pain at night, fewer disrupted positions)
- Functional capacity (easier stair climbing, sitting longer at desk)
- Activity tolerance (walking further, returning to short jogs)
- Confidence in movement (less fear of flare-ups)
At Head2Toe, physiotherapists often re-measure objective markers at follow-ups—range of motion, balance time, and strength tests—to demonstrate change you can see. This evidence-based approach means your progress is documented, not assumed.
Plateaus or minor setbacks are common and usually managed by adjusting load, exercise type, or treatment frequency. These aren’t failures; they’re part of the collaborative process of managing chronic conditions or complex injuries.

Follow-Up Appointments: How Often and What Happens
Physiotherapy is a process, not a one-off physio appointment. Follow-up sessions are crucial for safe progress and preventing setbacks.
Initial frequency: Many patients are reviewed twice weekly for 1–2 weeks, with frequency reducing as symptoms settle and self-management improves. A typical follow-up lasts 20 minutes—shorter than the initial consultation but focused on treatment and progression.
What happens in a typical follow-up:
- Review of symptom changes since last session
- Re-check of key tests (strength, movement, function)
- Progression or regression of exercises based on response
- Additional hands on treatment if indicated
- Discussion of activity levels and any concerns
Follow-ups help prevent compensating with other body parts (which can cause secondary problems), reduce the risk of re-injury, and refine goals. As you improve, focus might shift from basic walking to running or sport-specific drills.
At Head2Toe, your physio may suggest transitioning into physiotherapist-led Clinical Pilates or small-group rehab once pain is stable and the focus shifts to building long-term strength. This supports improving mobility and resilience beyond initial pain management.
Activity, Work, and Sport After Your First Session
Patients usually leave the initial consultation with specific advice about work duties, driving, housework, sport, and gym activity. This isn’t generic guidance—it’s based on your medical history, past injuries, and current presentation.
For office workers:
- Take posture breaks every 30–60 minutes
- Consider temporary ergonomic changes (monitor height, chair support)
- Limit prolonged sitting periods in the first week if aggravating
- Discuss sleeping positions if relevant to your condition
For active people and athletes:
- Swap running for walking or cycling in the first 1–2 weeks
- Avoid deep squats or heavy lifting until cleared
- Modify training intensity rather than stopping completely
- Communicate with your trainer about current restrictions
Complete rest is rarely recommended. Instead, activity modification keeps the injured area within an acceptable pain threshold—activity that doesn’t cause flare-ups lasting more than 24–48 hours.
If work restrictions or medical certificates are needed (e.g., modified duties for a warehouse role), your physio can provide documentation and liaise with employers where appropriate. This supports your return to daily life without unnecessary delays.
When and How We Coordinate With Podiatry or Other Services
Head2Toe offers integrated physiotherapy, podiatry, and clinical Pilates across its Melbourne clinics, so post-consult care can be coordinated when needed. This multidisciplinary approach addresses the body as a connected system.
Situations where podiatry referral might follow your initial physiotherapy assessment:
- Recurring plantar heel pain not responding to exercise alone
- Achilles issues linked to foot mechanics
- Running-related knee pain potentially caused by poor foot alignment
- Persistent shin splints requiring gait analysis
- Footwear concerns affecting lower limb function
Podiatrists may provide gait analysis, footwear advice, or custom orthotics to support the physio’s load-management plan. This coordination means potential contributing factors from the foot and ankle are addressed alongside your primary treatment techniques.
For certain conditions, patients progress onto physio-led Clinical Pilates programs (reformer-based, maximum 5 per class) once acute pain is controlled. This transition supports long-term strength, core control, and injury prevention—moving beyond relieve pain goals toward sustainable resilience.
This multidisciplinary model helps ensure long-term results rather than just short-term symptom relief.
When to Contact Your Physiotherapist Between Appointments
You don’t need to “tough it out” alone between sessions. Support is available via phone or email, and reaching out is encouraged.
Red flags requiring prompt contact:
- Significant new swelling
- New numbness or tingling
- Inability to bear weight that wasn’t present before
- Any symptoms that feel distinctly different or worse lasting 48-72 hours
Less urgent but important reasons to review with your physio:
- Uncertainty about how to perform an exercise correctly
- Repeated flare-ups after a specific activity
- Feeling the program is too easy or too hard
- Questions about whether an activity is safe to resume
Your physio can often make small adjustments remotely—changing exercise sets/reps or substituting movements—to keep progress on track until your next in-person review. This prevents weeks of frustration or setback.
Asking questions is part of an effective, collaborative process. Your physiotherapist understand that recovery involves ongoing communication, not just clinic visits. Feel confident reaching out whenever you’re unsure about your pain experience or program.
How Head2Toe Physiotherapy & Podiatry Supports Long-Term Results
At Head2Toe, the goal is helping patients get better, stay better, and live better—not just easing symptoms for a few days. This philosophy shapes everything from the initial consultation through to discharge and beyond.
What sets the approach apart:
- Emphasis on getting an accurate diagnosis
- Evidence-based protocols guiding each stage of rehab
- Clear outcome measures tracked at every follow-up
- Structured progression from acute pain to long-term strength
- Wear comfortable, loose fitting clothes for easy movement during sessions
Once your initial injury has resolved, options exist for ongoing preventative care:
- Periodic physio check-ins for maintenance
- Strength programs targeting identified weaknesses
- Clinical Pilates for core stability and body control
- Podiatry reviews for running or walking loads
- Lifestyle habits coaching for long-term health background
For readers in suburbs like Moonee Ponds, Brunswick, Kew, and Pascoe Vale—book your first physio appointment with confidence knowing a structured “after” plan is already built into the initial consultation.
The ultimate goal is confident self-management and resilience. You should return to work, sport, and daily life without relying on endless passive treatment. That’s what sustainable recovery looks like.

Frequently Asked Questions
How sore is normal after my first physio session?
Mild muscle soreness or stiffness for up to 24–48 hours after manual therapy or new exercises is common and usually safe. This is similar to post-workout soreness and indicates your tissues are responding to treatment.
Pain should gradually settle rather than intensify. If it becomes sharp, severe, or continues to worsen after 48 hours, contact the clinic for guidance.
Practical tips for managing post-session soreness include gentle movement (walking, light stretching), applying heat or ice if recommended by your physio, and avoiding sudden spikes in activity immediately after your first appointment. Bring clothing that allows easy access to the treatment area for future sessions.
Will I always need ongoing weekly physio appointments?
Weekly physiotherapy session schedules are sometimes useful early on, but frequency typically reduces as pain decreases and you become more independent with exercises. The adaptation phase requires closer monitoring; the later stages often don’t.
Some people only need a handful of sessions for straightforward conditions. Others with complex, chronic, or longer-standing issues may benefit from a longer—but less frequent—review schedule.
At Head2Toe, the number of sessions is based on your achievable goals, response to treatment, and objective progress. There’s no fixed pre-set package; your plan adjusts as you improve. If x rays or referral letters from previous assessments exist, these inform the timeline.
What if I miss a few days of my exercises?
Missing the occasional day isn’t a disaster, but consistent adherence over weeks is important for meaningful change. Think of it like training—sporadic effort produces sporadic results.
If you miss a few days, simply resume your program at the prescribed level rather than trying to “make up” missed sets all at once. Overloading to compensate often leads to flare-ups.
If you repeatedly struggle to fit exercises in, discuss time-efficient alternatives or habit strategies with your physiotherapist. A 10-minute routine done consistently beats a 30-minute routine that never happens.
Can I keep seeing my gym trainer or doing classes while in physio?
In many cases, it’s safe and beneficial to continue some form of training. Exercise supports recovery when appropriately managed. The key is ensuring your physio and trainer communicate about load and movement restrictions.
Share your physio’s guidelines with your trainer or class instructor—for example, “no heavy squats for 2 weeks” or “avoid impact landing exercises.” Most trainers appreciate this clarity and can modify sessions accordingly.
For certain acute injuries or post-surgery, your physio may temporarily advise pausing specific classes until movement control and tissue healing improve. This isn’t permanent—just strategic timing for managing chronic pain or acute conditions.
What if I don’t feel any improvement after a few sessions?
If there’s little or no progress after roughly 3 sessions, your physiotherapist will usually re-assess, adjust the plan, or consider further investigations such as imaging. Lack of progress isn’t ignored—it prompts a conversation.
Be open about your concerns. Expectations, goals, and home routines can all be reviewed together. Sometimes small adjustments—different exercises, modified intensity, or addressing lifestyle habits—unlock progress that wasn’t happening before.
In some complex cases, collaborative care with podiatry, your GP, or other specialists may be recommended. This multidisciplinary approach ensures nothing is missed and moves your recovery forward. Book your appointment today if you’re ready to begin your recovery with a team that supports you through every stage.







